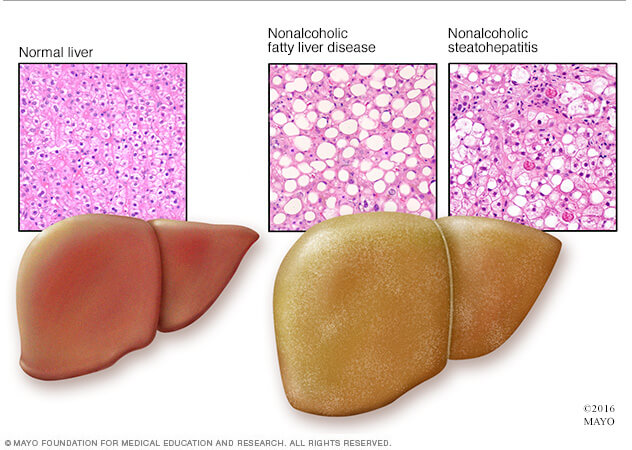
Non-alcoholic fatty liver disease is on the rise. Non-alcoholic fatty liver disease (NAFLD) is an inflammation of the liver caused by an accumulation of fat deposits in liver tissue. Today, “fatty liver” closely mirrors the global epidemics of obesity and type 2 diabetes.
Since its first description in the early 1980s as “a poorly understood and hitherto unnamed liver disease,” NAFLD is now considered to be the most common liver disease in the western world. A recent article appearing in the Journal of Hepatology estimates its prevalence in the U.S. general population between 25-46%, and up to 28% of obese children.
NAFLD has no approved pharmacological therapy. In other words, there are no drugs to treat this disorder, and alarmingly, the number of cases is expected to exceed over 100 million by 2030 unless lifestyle changes occur.
In individual cases, if NAFLD progresses past the inflammatory stage it can lead to scarring, fibrosis, oxidative and mitochondrial damage and eventually cirrhosis of the liver tissue, resulting in a more severe condition called non-alcoholic steatohepatitis (NASH). It has been estimated that 5-8% of NASH patients develop cirrhosis within five years, making NASH the third leading indication for liver transplantation in the U.S.
NAFLD is often asymptomatic in the beginning. However, even in early stages, routine blood tests can reveal elevations in liver enzymes known as GGT, ALT, and AST. Additionally, often present are markedly elevated triglycerides, low HDL cholesterol, elevated fasting insulin, elevated hbA1C, increased fasting blood glucose, and low testosterone in men. In some cases, an ultrasound examination of the liver may be warranted.
Known risk factors for developing NAFLD include:
- Obesity (a BMI over 30 and/or waist circumference more than 1/2 their height);
- Type 2 diabetes and insulin resistance;
- Lack of physical activity (sedentary lifestyle);
- Diet high in processed grains, fructose, fast food, and sugar-sweetened drinks;
- Hypothyroidism;
- Low testosterone in men;
- Polycystic ovary disease in women;
- Sleep apnea;
- Chronic hepatitis C;
- Celiac disease;
- Phosphatidylcholine and NAD deficiency;
- Genetic variants in the PEMT, PNPLA3, MTHFD1, and MTHFR genes;
- Leaky gut syndrome.
The good news is there are several ways to reverse and even completely resolve NAFLD if caught early.
The single best way is to lose weight. A 3-5% body weight loss will reduce steatosis. Both aerobic and resistance exercise a minimum of 150 minutes per week is also very beneficial. There is also ample, science-based evidence that certain nutritional supplements help, including the following:
- phosphatidycholine (750 mg/day)
- berberine (750 mg/day)
- curcumin (phytosome; 500 mg/ 2xday)
- vitamin E (500-800 IU daily)
- silybin (phytosome) or milk thistle (180 mg/day)
- pantethine (500-750 mg/day)
- NAC (1200 mg/day)
- alpha lipoic acid (300-600 mg/day)
- melatonin (3-20 mg/day)
- betaine or trimethylglycine (TMG; 500 mg/day)
- prebiotics such as inulin and probiotics
- nicotinamide riboside (100 mg/day)
Prevention through exercise and diet is the primary way to alleviate this growing epidemic, and it is never too late to start. As with any treatment protocol, it is important to consult your health care provider before beginning a supplementation program such as this.
Dr. John Dixon can be reached at the Natural Medicine Group (760) 345.7300.
References available upon request.